StoCastic | E-Triage: E-Triage
by Eric Hamrock
E-Triage supports emergency department triage decision-making to improve risk-stratification and decrease patient waiting
Towson, MD United States Emergency Medicine BigData AMIA2019 challenge AMIA2019 Finalists challengeAbout our project

The problem we solve: Increases in annual visits to US emergency departments (ED) to over 140 million have led to unprecedented levels of crowding and delays in care. Evidence linking pro-longed waits to adverse patient outcomes across many clinical conditions continue to mount. EDs have a need to execute front-end triage systems that can accurately identify patients with time-sensitive conditions from those with less urgent needs. Further triage processes have begun to shift for dual purposes: to drive efficient and cost-effective care trajectories. Safely supporting streaming operational models is difficult because accurately classifying many non-urgent patients, and atypically presenting high-risk patients, is only certain after thorough ED-based evaluation. Current standards for triage (Emergency Severity Index [ESI]) in the US consistently promote triage of a heterogeneous majority to mid-acuity Level 3, counter to the objective of triage. ESI no longer supports new and needed operational models.
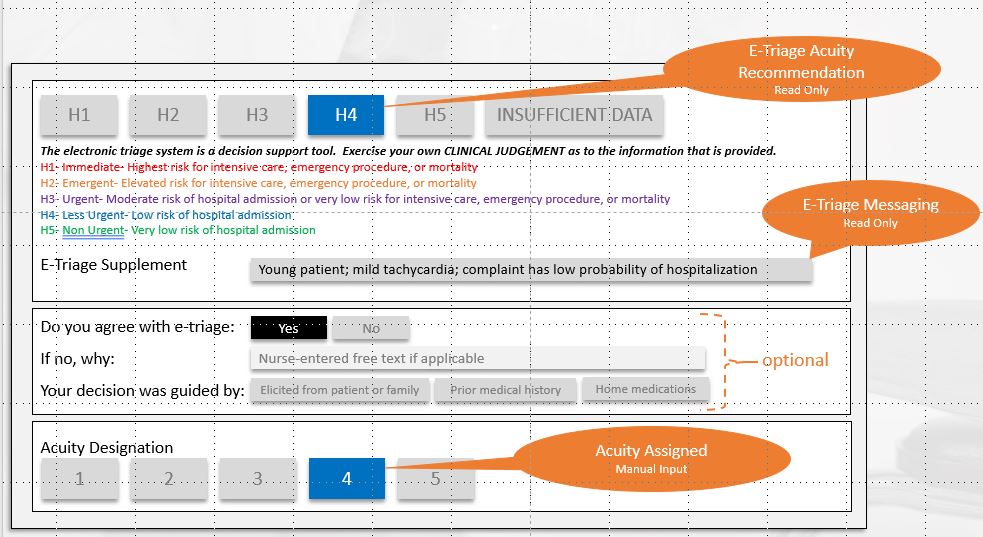
About our solution: The e-triage value proposition is to provide data-driven decision support for patient triage that is embedded within an ED’s local electronic health record (EHR) system or deployed on-line. Compared to ESI, we have demonstrated e-triage’s improved performance in distinguishing high-risk patients using multiple ED populations through both retrospective and prospective evaluation. More important from a financial and operational perspective is e-triage’s ability to improve recognition of low-risk patients safe for fast-track (non-urgent care). The objective of identifying and streaming non-urgent patients is to: (1) reduce ED crowding, (2) minimize non-urgent patient waiting, and (3) prevent resource over-utilization that plagues this costly care setting.
Progress to date:
E-Triage is deployed in 4 emergency departments (ED). We have conducted numerous peer-reviewed and published studies on E-Triage. We are currently realizing revenue for E-Triage and are seeking additional partners to implement.
About Our Team

Creator: Eric Hamrock
Location: Maryland
Bio: Eric is a healthcare leader with over 17 years of experience in operational leadership, performance improvement, and project management. Eric is a Certified Lean Sigma Black Belt with a track record of implementing initiatives focused on operational and financial performance in the healthcare industry including Johns Hopkins Medicine and Sunrise Senior Living with measurable results.
Title: Co-Founder/CEO
About Team Members
Scott Levin
Co-Founder/CTO, PhD
Biography: Scott is an Associate Professor and Associate Director for Research in Emergency Medicine, at the Johns Hopkins University. He also serves as the Systems Director for the Malone Center for Engineering in Healthcare at the Johns Hopkins University. He holds a PhD in Biomedical Engineering from Vanderbilt University. Scott has 15+ years development of health systems engineering software focused on healthcare value and medical decision-making.
Title: Co-Founder/CTO
Advanced Degree(s): PhD
LinkedIn:
https://www.linkedin.com/in/scott-levin-a49a2995/
Jeremiah Hinson
Chief Medical Officer, MD, PhD
Biography: Jeremiah Hinson is an Assistant Professor and Director of Residency Research for Emergency Medicine at Johns Hopkins University. He holds an MD from Albert Einstein College of Medicine and PhD in Molecular and Cellular Pathology from the University of North Carolina. Dr. Hinson's experience is in improvement of patient outcomes using data-driven methods focused on emergency department operations, acute kidney injury, and infectious disease.
Title: Chief Medical Officer
Advanced Degree(s): MD, PhD
About Our Company
Location: 7400 York Road
222
Towson, MD 21024
US
Founded: 2015
Website: https://www.stocastic.com
Product Stage: In the Market
Employees: 10-20
How We Help Patients
E-Triage attacks the problem of ED crowding and wait time. We have shown an ability to improve the ED wait time at our client Emergency Departments through using evidence based methods.
How We Help Physicians
E-Triage helps providers by providing operational decision support mainly for triage nurses. The current standard of the Emergency Severity Index has proven to be highly subjective and based upon estimated resources. E-Triage combines clinical judgement with evidence to support improved identification of patients' at risk for critical care and hospitalization.
How We Help Hospitals
E-Triage has proven to create 10,000 bed hours in an average ED. This is equivalent to cost savings of approximately $674,000 per year thus helping to bend the cost curve by providing better outcomes with the same resources.
How We Help Partners
E-Triage can provide real time operational decisioin support for identifying patients at risk for critical outcomes or admission. StoCastic also has a deep level of exerience in taking evidence based operations research tools to the bedside.
Challenge Mission
Affiliation(s)
Scott Levin, PhD is an Associate Professor and Associate Director for Research in Emergency Medicine at Johns Hopkins Unversity. He is also the Director for Systems in the Malone Center for Engineering in Healthcare at Johns Hopkins University.
Jeremiah Hinson, MD, PhD is an Assistant Professor and Director of Residency Research in Emergency Medicine at Johns Hopkins University.
Johns Hopkins University also maintains a minority equity position in StoCastic.
Key Milestones Achieved and Planned
Our Competitive Advantages
E-Triage is currently under a provisional patent. Through market research and customer discovery we have not seen another product addressing ED crowding with a triage tool using a similar approach. We describe competitive risks in the competitors section.
Barriers to Entry
Patent for E-Triage.
Partnership with Johns Hopkins Medicine provides a competitive advantage.
Have demonstrated evidence of success in deploying E-Triage within EHR systems achieving improvements in patient flow linked to cost-savings and/or revenue generation.
Funding, Partners and Alliances To Date
Our current source of external funding has been through the NSF SBIR program. We are currently within our Phase II and have raised ~$830K to date.
Revenue
Our annual revenue ranges between $250-500K per year. A portion of this is SaaS ARR and the rest is from R&D funding (i.e. grants, partner funding) and consulting revenue.
Innovation Details
Intellectual Property Summary
Clinical Information
E-Triage has been peer reviewed through the following publications.
Regulatory Status
We have recieved guidance from an FDA consultant and are continuously monitoring the regulatory landscape. We are considering applying for FDA clearance for future claims and iterations of StoCastic products in the near future.
How we will use the funds raised
The funding will enable to StoCastic to further deploy E-Triage and to improve it's functionality to other health systems. We will use this funding to support further data science resources and to invest in marketing and sales resources. This funding will allow improved functionality for future iterations of E-Triage and to create further awareness of the tool through the participation in conferences both academic and industry related.
Thank You
If you or a loved one has every had to wait in an emergency department you know how frustrating the experience and wait can be. E-Triage is an evidence based tool that leverages the data that health systems have invested significant amounts of money into but have not realized the benefits that were anticipated. StoCastic has realized significant results in some of the world's leading hospitals and would like to spread this work to the rest of the world including your community emergency department.
Updates
No updates found .
Supporters
-
, DO
11/05/2019 - Liked the project.
11/03/2019 - Interested in trying the project.
11/03/2019 - Followed the project.
11/01/2019 - Followed the project.
10/30/2019 - Backed the project for $50
10/30/2019 - Liked the project.
10/30/2019 - Followed the project.
10/29/2019 - Liked the project.
10/26/2019 - Liked the project.
10/24/2019 - Liked the project.
10/24/2019 - Followed the project.
10/24/2019 - Liked the project.
10/22/2019 - Liked the project. Instant Feedback
Instant Feedback
Help us find best new ideas to fund by telling us what you think. Your feedback goes straight to the team behind this project in private, so tell them what you really think.
58Medstartr
Index Score53
Interest
Score1
Adoption
Score10
Likes0
Partners0
Pilots5
Follows-
This campaign has ended but you can still get involved.See options below.
$50 pledged of $25,000 goal
Instant Feedback
Help us find best new ideas to fund by telling us what you think. Your feedback goes straight to the team behind this project in private, so tell them what you really think.



